

About Pediatric Cancers
Cancer in children is rare. The majority of malignancies (99%) occur in adults, while older persons are more frequently affected. One in three people will develop cancer at some point in their lives, compared to one in 285 children who will do so before turning 20. Children can acquire cancer in any region of the body, including the lymphatic and blood systems, the brain and spinal cord (central nervous system, or CNS), the kidneys, and other organs and tissues.


Symptoms & Signs
- Unexpected weight drop.
- Headaches, frequently accompanied by morning vomiting.
- Increased inflammation or ongoing discomfort in the legs, back, joints, or bones.
- Severe bruising, bleeding, or rash development.
- Infections that recur frequently or are chronic.
- An off-white hue behind the pupil.
- Persistent nausea or vomiting without feeling sick.
- Persistent fatigue or a pronounced paleness.
- Rapid and persistent alterations in the eyes or vision.
- Unknown origin recurrent or chronic fevers.
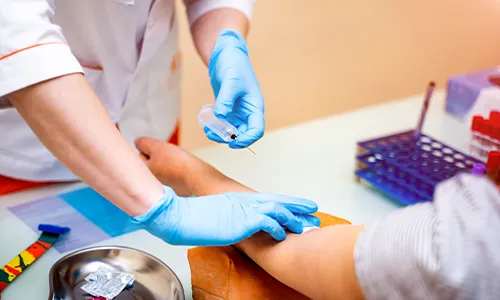

Diagnosis
Pediatric cancers diagnostic tests determine whether you have the disease and how aggressive it may be.
Tools and tests include:
- Blood tests
- CT or CAT scan
- PET-CT scan
- Lumbar puncture (spinal tap)
- Ultrasound
- MRI
- Bone marrow aspiration
- Biopsy
- Scans or radioisotope studies


Sub-Types
Leukemia
- Acute lymphoblastic leukemia (ALL)
- Acute myeloid leukemia (AML)
Brain and spinal cord tumors
A. Glial tumors
- Astrocytoma
- Oligodendroglioma
- Ependymoma
- Choroid plexus carcinoma
- OligoastrocytomaGlioblastoma
B. Mixed glial neuronal tumors
- Ganglioglioma
- Astrocytoma
- Desmoplastic infantile ganglioglioma
- Pleomorphioc xanthoastrocytoma
- Anaplastic ganglioglioma
C. Neural tumors
- Gangliocytoma
- Neurocytoma
D. Embryonal tumors
- Medulloblastoma
- Medulloepithelioma
E. Ependymoblastoma
- Atypical Teratoid/Rhabdoid tumor
F. Pineal tumors
- Pineocytoma
- Neuroblastoma
- Non-Hodgkin lymphoma
- Hodgkin lymphoma
- Hepatoblastoma
- Hepatocellular carcinoma
- Pleuropulmonary blastoma
- Osteosarcoma
- Ewing sarcoma
- Germ cell tumors
- Rhabdomyosarcoma
- Wilms tumor


Treatment Modalities
a. Surgical Oncology
- Surgery is the removal during an operation of the tumor, whether it be cancerous or not, along with a tiny portion of the surrounding healthy tissue. Surgery is a common component of the treatment for many kids with tumors.
- The medical professionals who specialize in operating to remove tumors include surgical oncologists, pediatric surgeons, and neurosurgeons.
b. Medical Oncology
- Chemotherapy- Chemotherapy kills cancer cells by using chemicals. One chemotherapy medicine may be administered, or two or more drugs may be combined.
- Targeted Therapy- For the treatment of advanced endometrial cancer, targeted medication therapy is frequently used in conjunction with chemotherapy.
- Immunotherapy- A medicinal therapy called immunotherapy supports the immune system’s ability to fight cancer. If the cancer is advanced and other treatments have failed for endometrial cancer, immunotherapy may be tried.
c. Radiation Oncology
- To kill cancer cells, radiation therapy employs powerful energy beams like protons and X-rays. Radiation from a machine outside of your body or radiation implanted inside of your body can both be used in radiation therapy.


Coping with Treatment
Along with the medical side effects of pediatric cancer therapy, patients also deal with the financial burden of cancer care and the emotional and social impacts. Talking to a counselor, or family member can help them to cope with treatment. MOC provides facility of psycho Onco-Counseling and Nutritional counseling to help patients.


Post Treatment Support
Post-treatment pediatric cancer survivors can go through long-term side effects of surgery, radiation therapy, chemotherapy, and hormonal therapy. They can also have symptoms such as headaches, hair loss, nausea, vomiting, extreme tiredness (fatigue), hearing loss, and cataracts. Survivors require empathy, mental strength, and support from their families, they can also join pediatric cancer Post-Treatment Survivorship Support Groups.


Follow-ups Cancer Care Plan
Post-treatment one must request a follow-up treatment plan. Doctors provide a personalized treatment plan based on the type and stage of cancer.


Surveillance and monitoring for Signs & Symptoms of Recurrence
One aim of follow-up care is checking for a recurrence. One should never miss follow-up visits and never ignore any symptoms of recurrence. Because some cancer cells may remain undiscovered in the body in small locations that don’t respond to treatment, cancer can reoccur. A physician who is knowledgeable about your medical history can provide you with personalized information regarding your risk of recurrence during follow-up care


Specialized Doctors at M | O | C
Find the nearest center
Cancer Centres
Mumbai
Pune
Other Locations
Cancer Clinics
Borivali
+91 9920767626
Book Your Appointment



























.png)











.png)



